Birth Control Pills: Effectiveness, Side Effects, and Key Interactions
To get started, it helps to know what we're talking about. Birth control pills are hormonal medications taken daily to prevent pregnancy by regulating the reproductive cycle. They are often referred to as oral contraceptives or OCPs. While their main job is stopping pregnancy, many people use them to manage acne, painful periods, or endometriosis.
The Two Main Types of Pills
Not all pills are created equal. Depending on your health history, your doctor will likely steer you toward one of two categories. The first is Combined Oral Contraceptives (COCs). These contain two hormones: estrogen and progestin. They work by stopping ovulation-meaning your ovaries don't release an egg. Most modern COCs use a low dose of estrogen (usually under 50 µg) to keep the risk of blood clots low while staying effective. A common example is the combination of ethinyl estradiol and levonorgestrel.
The second type is the Progestin-Only Pill (POP), often called the "mini-pill." These contain no estrogen, making them a safer bet for people who cannot take estrogen due to medical reasons or those who are breastfeeding. Unlike combined pills, some POPs have a very narrow window for timing; if you take it more than a few hours late, the effectiveness can drop significantly.
| Feature | Combined Pill (COC) | Mini-Pill (POP) |
|---|---|---|
| Hormones Used | Estrogen & Progestin | Progestin Only |
| Primary Action | Stops ovulation | Thickens cervical mucus |
| Timing Flexibility | Moderate (several hour window) | Strict (narrow window) |
| Common Use Case | General contraception, acne | Estrogen sensitivity, breastfeeding |
Why "Typical Use" Matters More Than "Perfect Use"
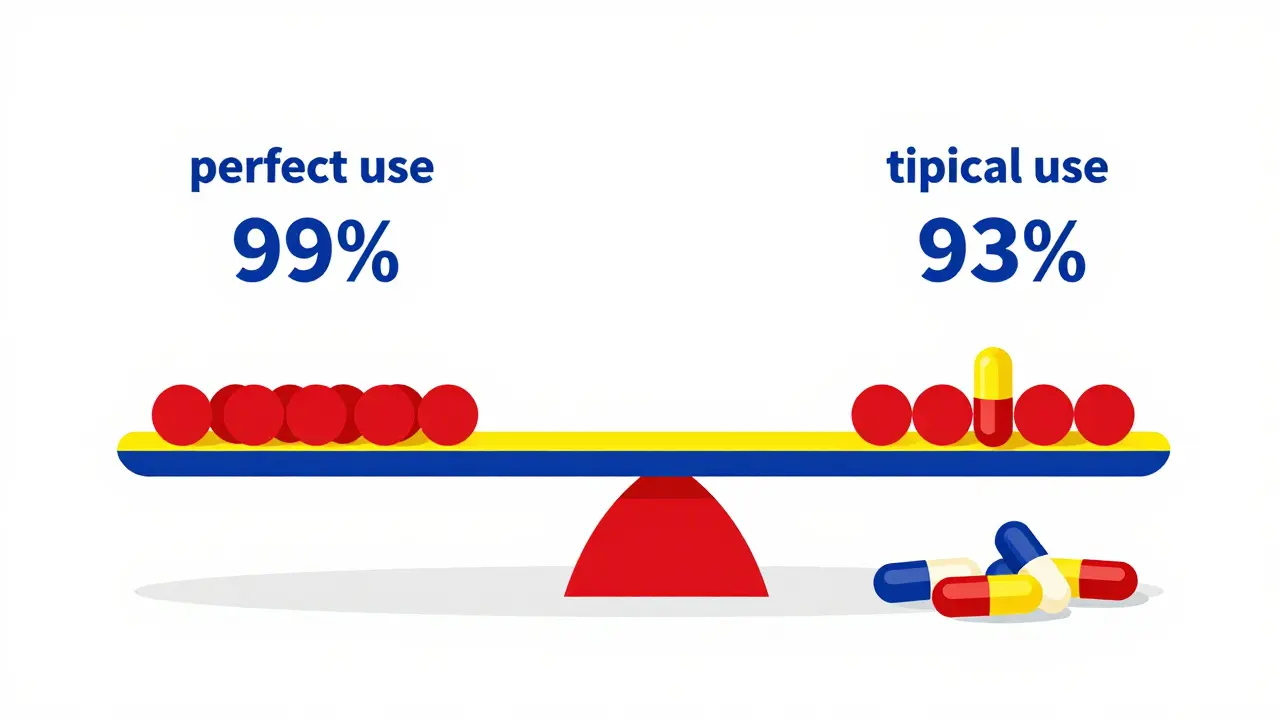
When you look at the packaging, the 99% effectiveness rate refers to "perfect use." This means the pill was taken at the exact same time every single day, with no missed doses, no vomiting or diarrhea, and no drug interactions. In reality, life happens. You forget a pill on a trip, or you sleep through your alarm.
This is where "typical use" comes in. For most people, the actual effectiveness is closer to 93%. This means about 7 out of 100 women using the pill will experience an unintended pregnancy within a year. Why is the gap so big? Because the pill requires a daily action. Compared to Long-Acting Reversible Contraceptives (LARCs) like IUDs or implants-which you "set and forget" for years-the pill is much more prone to human error. Research shows that younger users, specifically those under 21, face nearly double the pregnancy risk when using short-acting methods like the pill compared to older adults, simply because sticking to a strict daily routine is harder when your life is in transition.
Health Benefits Beyond Pregnancy Prevention
One of the biggest reasons people choose the pill over an IUD or a condom is that it does a lot more than just stop pregnancy. Because it regulates your hormones, it can turn a chaotic menstrual cycle into a predictable one. If you struggle with severe PMS or heavy bleeding, the pill can be a lifesaver.
There are also some serious long-term health wins. Data indicates that using combined pills can significantly lower the risk of certain cancers. For example, there is a documented 50% reduction in endometrial cancer risk, and a 27% reduction in ovarian cancer risk, with the protection actually increasing the longer you stay on the medication. For those dealing with hormonal acne, specific formulations containing drospirenone are FDA-approved to clear skin while providing contraception.
The Risks and Side Effects You Should Know
We can't talk about hormones without talking about risks. The most serious concern with combined pills is the risk of blood clots, which can lead to an ischemic stroke or myocardial infarction (heart attack). This risk is tied closely to the amount of estrogen in the pill. This is why the industry shifted away from the massive 10,000 µg doses used in the 1960s to the low-dose options we have today.
Beyond the serious stuff, there are common "nuisance" side effects. Some people experience breakthrough bleeding (spotting between periods), breast tenderness, or mood swings. Often, these side effects disappear after three to six months as the body adjusts to the new hormone levels. If they don't, switching to a different progestin type often solves the problem.
It is also crucial to remember a common mistake: Oral contraceptives do not protect you from sexually transmitted infections (STIs). If you have a new partner or multiple partners, the pill should be paired with condoms to ensure full protection.
Interactions: What Can Make the Pill Fail?
You might be taking your pill perfectly, but another medication could be canceling it out. Some drugs speed up the way your liver processes estrogen and progestin, essentially "flushing" the hormones out of your system before they can do their job. Certain antibiotics, some anti-seizure medications, and medications used to treat HIV can interfere with the pill's effectiveness.
St. John's Wort, a common herbal supplement for depression, is another known culprit that can lower the concentration of contraceptive hormones in your blood. If you are starting a new medication, always ask your pharmacist if it interacts with your specific brand of birth control. If there is an interaction, you'll need a backup method, like condoms, until you finish the other medication.
Practical Tips for Maximum Effectiveness
If you want to move from "typical use" (93%) to "perfect use" (99%), you need a system. Relying on memory is a gamble. Try these strategies:
- Tie it to a habit: Take your pill while brushing your teeth or right after your first cup of coffee.
- Use an app: There are dozens of pill-reminder apps that won't stop buzzing until you mark the dose as taken.
- Keep a backup pack: Always have an extra blister pack in your purse or car. If you realize you forgot a pill while you're out, you can take it immediately.
- The Seven-Day Rule: Remember that the pill can take up to a week to become fully effective. If you start on a day other than your first day of your period, use a backup method for the first seven days.
What happens if I miss one pill?
If you miss one dose of a combined pill, take it as soon as you remember, even if it means taking two pills in one day. You are generally still protected. However, if you miss two or more, your risk of ovulation increases. In that case, you should use a backup method like condoms for the next seven days.
Can birth control pills cause infertility?
No. Birth control pills do not cause permanent infertility. Once you stop taking them, your fertility typically returns almost immediately. Statistics show that 97% of women have a spontaneous period within 90 days of stopping the pill.
Which pill is the safest for my heart?
Generally, pills with lower doses of estrogen (under 30 µg) combined with levonorgestrel are considered to have a safer cardiovascular risk profile. If you have a history of high blood pressure or smoking, your doctor might recommend a progestin-only pill to avoid estrogen-related risks.
Do I need to take the placebo pills in the pack?
The placebo (reminder) pills do not contain hormones and don't prevent pregnancy. They exist to keep you in the habit of taking a pill every day so you don't forget to start your next active pack. If you forget a placebo pill, it doesn't affect your protection.
Can I take the pill if I have migraines?
It depends on the type of migraine. People who experience migraines with aura may be at a higher risk for stroke when taking estrogen-containing pills. In these cases, progestin-only options are usually the safer alternative. Always discuss your migraine history with your provider.