Fluoroquinolone Side Effects: Tendinopathy and Nerve Damage Risks
Fluoroquinolone Side Effect Risk Calculator
Assess Your Risk
This tool calculates your risk of tendon damage or nerve injury from fluoroquinolone antibiotics based on your health factors. It's not medical advice.
When you take an antibiotic to fight off an infection, you expect to feel better - not worse. But for some people, a common class of antibiotics called fluoroquinolones can trigger serious, sometimes permanent damage to tendons and nerves. These drugs - including ciprofloxacin, levofloxacin, and moxifloxacin - were once go-to treatments for everything from urinary infections to sinusitis. Now, they’re being pulled back from routine use because of the risks they carry. And if you’ve taken one recently, or are considering it, you need to know what to watch for.
What Are Fluoroquinolones?
Fluoroquinolones are a type of broad-spectrum antibiotic developed in the 1960s. They work by blocking bacteria from reproducing, and they’re good at getting into tissues - skin, lungs, urine, even bones. That made them popular. But their power came with hidden costs. The U.S. Food and Drug Administration (FDA) first added a black-box warning - its strongest alert - in 2008. By 2016, after reviewing thousands of reports, they made it clear: these drugs can cause disabling and potentially permanent side effects. The European Medicines Agency (EMA) followed in 2019, restricting their use to only the most serious infections when nothing else works.
Today, fluoroquinolones are no longer first-line treatments for common problems like uncomplicated urinary tract infections, acute bronchitis, or sinus infections. If you’re prescribed one for one of those, ask: Is there another option? Because for many people, the risks outweigh the benefits.
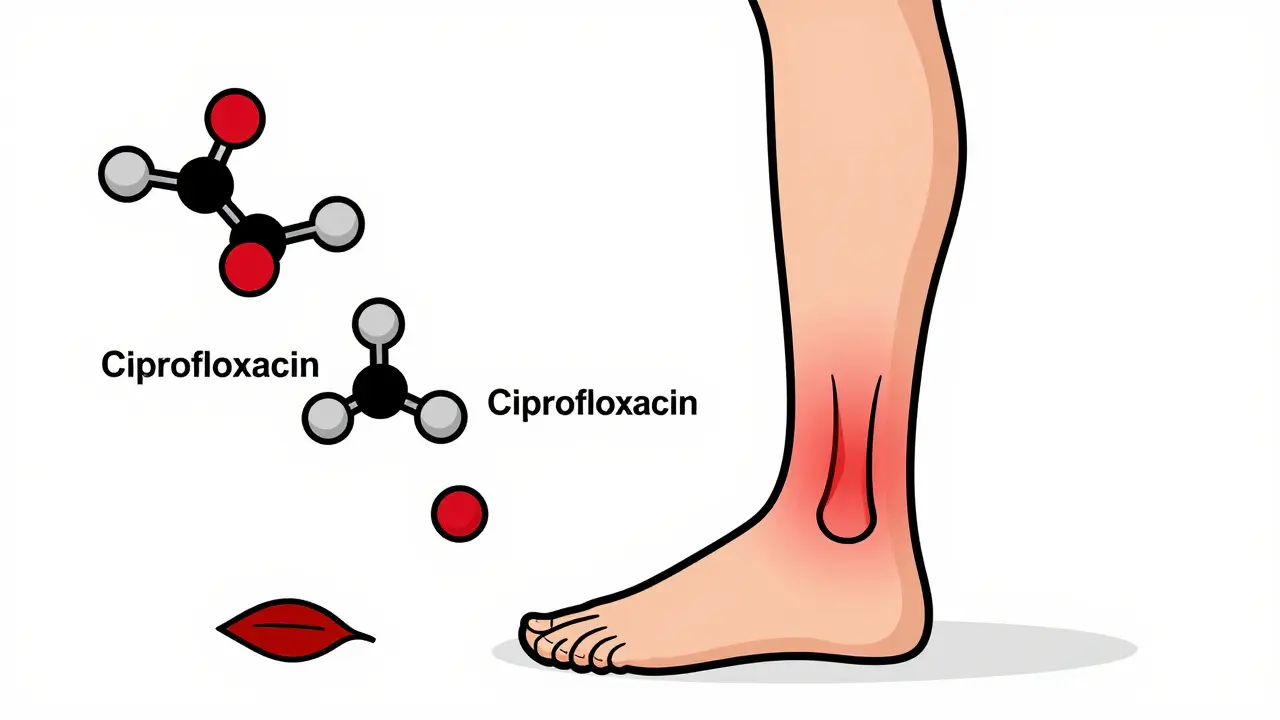
Tendinopathy: When Your Tendons Start to Fail
The most feared side effect of fluoroquinolones is tendinopathy - inflammation or rupture of tendons. The Achilles tendon, the thick band connecting your calf to your heel, is the most commonly affected. Studies show it’s involved in nearly 90% of cases. But other tendons - like the rotator cuff in your shoulder or the one in your wrist - can also be damaged.
The numbers are alarming:
- Between 0.14% and 0.4% of people taking these drugs develop tendinopathy - rare, but serious.
- Up to 40% of those cases turn into full tendon ruptures.
- Half of all tendon injuries happen after you’ve stopped taking the antibiotic.
- Symptoms can appear as early as 2 days after starting the drug - or as late as 152 days later.
And it doesn’t just happen to older people. While those over 60 are at higher risk - with a 2.7 times greater chance of rupture - younger adults aren’t immune. The real danger spikes when you combine fluoroquinolones with corticosteroids. That mix increases your risk of tendon rupture by 46 times. That’s not a typo. A single course of prednisone on top of ciprofloxacin can turn a routine infection treatment into a life-altering injury.
Signs to watch for:
- Sudden, sharp pain in a tendon - especially the heel, shoulder, or wrist
- Swelling or thickening around the tendon
- Difficulty walking, lifting, or moving the affected limb
- Pain that gets worse with activity
One patient in Bristol described it this way: "I was walking my dog, and my right Achilles just gave out. No warning. No trauma. Just… snap." He was on levofloxacin for a mild respiratory infection. He needed surgery. Took 11 months to walk normally again.
Nerve Damage: The Silent Threat
Alongside tendon damage, fluoroquinolones can attack nerves - a condition called peripheral neuropathy. This isn’t just numbness. It’s burning, tingling, electric shocks, or a feeling like you’re walking on glass. It can start within days of taking the drug and may not go away.
Studies show about 4.3% of patients develop symptoms. That might sound low, but for those affected, it’s devastating. In one study, 10% of patients with fluoroquinolone-induced neuropathy still had pain, weakness, or loss of sensation two years later. Some never fully recover.
What makes this worse? The delay. Many patients don’t connect their nerve pain to the antibiotic they took weeks or months earlier. Their doctor might blame it on diabetes, aging, or "just stress." By the time it’s recognized, the damage may already be done.
Key signs of nerve damage:
- Shooting or burning pain in hands or feet
- Numbness or "pins and needles" that doesn’t go away
- Weakness in arms or legs
- Loss of balance or coordination
There’s no cure. Stopping the drug helps - but doesn’t guarantee recovery. Some people need physical therapy. Others live with chronic pain.
Who’s at Highest Risk?
Not everyone gets these side effects. But certain factors make it much more likely:
- Age 60+: 38% of reported tendon injuries happen in this group.
- On corticosteroids: The combination is a recipe for disaster. Avoid both together at all costs.
- Diabetes: Poor blood sugar control weakens tendons and nerves.
- Previous tendon injury: If you’ve torn a tendon before, you’re more likely to do it again.
- Kidney problems: The body can’t clear the drug properly, leading to higher levels in tissues.
And here’s something many don’t realize: you don’t have to be on the drug long. A 7-day course is enough. In fact, half of all tendon ruptures happen within the first week. One study found 85% of cases occurred within 30 days - even after stopping the medication.
How Common Is This? The Real Numbers
Regulatory agencies say these side effects are "rare." But "rare" doesn’t mean "impossible." And when the damage is permanent, even one case is too many.
Here’s what the data shows:
- Fluoroquinolones increase the risk of Achilles tendon rupture by 4.1 times compared to other antibiotics.
- For every 1,301 courses of fluoroquinolones prescribed, one extra case of aortic aneurysm or dissection occurs - another serious, life-threatening risk.
- On Drugs.com, ciprofloxacin has a 2.2 out of 5 rating, with 68% of negative reviews citing tendon or nerve damage.
- The Fluoroquinolone Effects Research Foundation has over 8,500 patient reports - 78% of them involving tendon problems.
These aren’t outliers. They’re patterns. And they’re growing. Since 2016, prescriptions for fluoroquinolones in the U.S. have dropped by over 70% for mild infections. But they’re still being used - often unnecessarily.
What Should You Do?
If you’re currently taking a fluoroquinolone:
- Stop immediately if you feel pain, swelling, or tingling in a tendon or nerve.
- Don’t wait. Don’t assume it’s "just soreness."
- Call your doctor - but be specific: "I think this might be a fluoroquinolone side effect."
- Avoid corticosteroids completely. Even a short course can trigger rupture.
- Rest the affected area. Don’t push through pain.
If you’ve taken one in the past and are now experiencing symptoms - even months later - get evaluated. Many doctors still don’t know to look for this. Bring printouts of the FDA or MHRA warnings. Ask for a referral to a specialist in musculoskeletal or neurological disorders.
Alternatives Exist
For most infections, there are safer choices:
- Uncomplicated UTIs: Nitrofurantoin or trimethoprim
- Sinus infections: Amoxicillin or doxycycline
- Respiratory infections: Azithromycin or amoxicillin-clavulanate
These alternatives don’t carry the same risks. They may take a little longer to work, or require a different dosage - but they’re far safer. Ask your doctor: "Is this the safest option?" If they say yes - great. If they hesitate - push back.
The Bigger Picture
Fluoroquinolones aren’t going away. They still have a vital role - for life-threatening infections like anthrax, complicated pneumonia, or severe kidney infections where no other drugs work. But their use in everyday situations is outdated. The risks are too high.
Regulators know this. The UK’s MHRA, the FDA, and the EMA all agree: these drugs should be reserved for when there’s no alternative. Yet, doctors still prescribe them. Why? Habit. Convenience. Lack of awareness.
You have the right to ask questions. You have the right to refuse. And if you’ve been injured by one of these drugs, you’re not alone. Tens of thousands of people are living with tendon pain, nerve damage, and chronic disability because they were never warned.
Knowledge is your best defense. Don’t wait until it’s too late.
Can fluoroquinolone side effects be reversed?
In some cases, stopping the drug early can prevent permanent damage. But if tendinopathy or nerve damage has already occurred, recovery isn’t guaranteed. Tendon ruptures often require surgery and months of rehab. Nerve damage can persist for years - or become permanent. The sooner you stop the drug at the first sign of symptoms, the better your chances. But there’s no cure for the damage already done.
How long after taking fluoroquinolones can side effects appear?
Symptoms can show up as early as 2 days after starting the drug - or as late as 152 days after stopping. Half of all tendon injuries happen after the course is finished. This delay is why many patients and doctors miss the connection. If you’ve taken a fluoroquinolone in the past few months and now have unexplained pain or numbness, consider it a possible side effect.
Are some fluoroquinolones riskier than others?
Yes. Ciprofloxacin is the most commonly linked to tendon damage, followed by levofloxacin and moxifloxacin. But all fluoroquinolones carry the same black-box warning from the FDA. No one is safe. Even if you’ve taken one before without issues, that doesn’t mean you’re immune. Risk increases with age, steroid use, and kidney problems - not past tolerance.
Why are these drugs still available if they’re so dangerous?
They’re still necessary for life-threatening infections where alternatives don’t work - like hospital-acquired pneumonia, complicated UTIs, or anthrax exposure. The problem is their overuse for minor infections. Regulations now restrict them to second-line use, but not all doctors follow the guidelines. That’s why patient awareness is critical.
What should I do if I think I’m having side effects?
Stop taking the drug immediately. Contact your doctor and say: "I believe I’m experiencing fluoroquinolone-induced tendinopathy or neuropathy." Request an evaluation for tendon inflammation or nerve damage. Avoid corticosteroids and strenuous activity. Document your symptoms and timeline. Consider seeking a second opinion from a specialist in rheumatology or neurology. Early action can prevent permanent damage.
Fluoroquinolones saved lives - but they also broke them. The medical community is catching up. Now it’s up to you to protect yourself.