How to Prevent Non-Adherence During Life Transitions or Stress
When your life changes - a new job, a move, a breakup, or even just a really rough few weeks - your medication routine doesn’t pause. But yours might. And that’s not because you’re lazy or careless. It’s because your brain is overloaded. Studies show that during major life transitions, medication adherence drops by an average of 32%. That’s not a small number. It’s the difference between staying stable and ending up back in the hospital.
Think about it: you used to take your pills every morning after brushing your teeth. Now you’re packing boxes, switching time zones, or sleeping on a friend’s couch. Your routine is gone. Your stress is up. Your attention is split. And suddenly, that pill bottle sits untouched for days. You’re not alone. In fact, 78% of people with chronic conditions admit they’ve skipped doses during a major life shift.
Why Your Routine Falls Apart When Life Changes
It’s not about willpower. It’s about structure. When your environment shifts - whether it’s a new city, a new schedule, or a new emotional state - your brain doesn’t automatically transfer old habits. It needs new anchors. Without them, even the most disciplined person forgets. Research from the Journal of Personality and Social Psychology found that maintaining just 3-5 daily anchor activities during transitions reduces psychological distress by 23% and improves medication adherence by over 31%.
Those anchors aren’t fancy. They’re simple: taking your pill right after you drink your first sip of coffee. Putting your pillbox next to your keys. Checking your meds before you lock the door. These are tiny rituals, but they’re the difference between remembering and forgetting.
And it’s not just about forgetting. Stress changes your brain chemistry. Cortisol spikes. Decision-making shuts down. You don’t think about your meds because your brain is screaming: "Survive this moment." That’s why reminder apps alone fail during transitions. They work fine when life is calm. But when you’re moving, grieving, or starting a new job? Those notifications get buried under 20 other urgent things.
The Three Lists That Keep You on Track
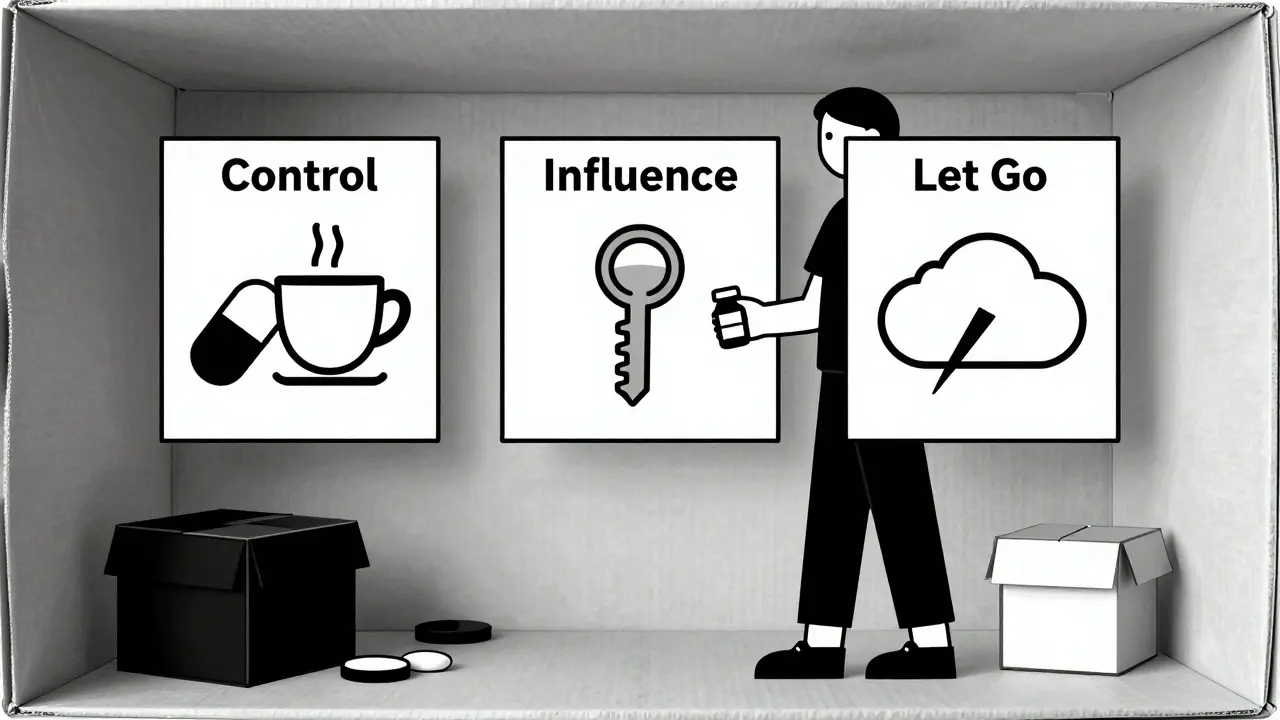
One of the most powerful tools for staying on track isn’t a tech app. It’s a piece of paper. Write down three lists:
- Things you can control directly (27.3% of transition stressors): When you take your pill, where you keep it, who reminds you, how you refill it.
- Things you can influence (43.8%): Talking to your doctor about adjusting your schedule, asking a friend to check in, choosing a pharmacy near your new home.
- Things outside your control (28.9%): Your boss’s schedule, your ex’s behavior, traffic delays, weather.
Here’s the trick: spend zero energy on the third list. Seriously. Don’t ruminate on it. Don’t stress about it. Redirect that mental energy into the first two. That shift alone has been shown to boost adherence by over 22% during upheaval.
For example: if you’re moving, you can’t control the moving truck being late. But you can control putting your meds in a labeled bag with your toiletries. You can’t control your new job’s hours. But you can control setting a daily alarm for 10 minutes after your first coffee break.
Flexible Routines Beat Rigid Schedules
Forget "take this at 8 a.m. sharp." That doesn’t work when your schedule is in flux. What does work? Time-blocking.
Instead of tying your pill to a clock, tie it to an action. Like:
- "After I brush my teeth."
- "Before I check my phone in the morning."
- "Right after I eat lunch."
A 2022 study from the Greater Boston Behavioral Health Institute found that people who used time-blocking - linking meds to behaviors, not clocks - improved adherence by 28.6% during transitions. Why? Because actions are more reliable than times. You’ll brush your teeth even if you’re tired. You’ll eat lunch even if your day is chaos.
Also, build in flexibility. If you’re traveling? Have a backup plan. Keep a 3-day supply in your bag. Set a reminder for when you land. Ask your doctor for a short-term prescription refill before you go. These aren’t extra steps - they’re survival tools.
Social Support Isn’t Optional - It’s Essential
People who feel supported during transitions are 34% more likely to stick with their meds. Not because they’re guilted. But because connection reduces stress. A 2022 study in Health Psychology found that perceived social support lowers cortisol levels by 41.7%. Less stress = better decision-making = better adherence.
So who can help?
- A friend who texts you every morning: "Did you take your pill?"
- A family member who picks up your prescription when you’re swamped.
- A support group where someone says, "I skipped my meds during my divorce too. Here’s what worked for me."
You don’t need to tell everyone. Just pick one or two people who get it. And be specific: "Can you remind me every Tuesday?" or "Can you help me find a pharmacy near me?"
Reddit’s r/ChronicIllness community is full of stories like this. One user wrote: "My sister started leaving sticky notes on my fridge with my pill times. I didn’t even realize I was forgetting until I saw them. Now I look for them every morning. It saved me."
Therapy Works - Especially ACT
Not all therapy is the same. If you’re struggling to stay on track during a transition, Acceptance and Commitment Therapy (ACT) has the strongest evidence. A 2022 JAMA Internal Medicine trial found that ACT improved adherence by 48.6% compared to standard care.
ACT doesn’t try to eliminate stress. It teaches you to carry it while still doing what matters. Instead of fighting the thought "I can’t handle this right now," you learn to say: "I’m overwhelmed. And I still need to take my pill."
It’s not about being positive. It’s about being present. And that’s exactly what adherence during chaos requires.
Why Apps Alone Fail - And What Actually Helps
Medication reminder apps work well when life is stable. But during transitions? Their advantage shrinks from 22.8% to just 8.3%. Why? Because they don’t adapt. They don’t ask: "Are you moving? Are you grieving? Are you working double shifts?"
That’s why apps like TransitionAdhere and LifeShiftRx are getting 4.2-star ratings - while general apps sit at 3.5. These tools let you map your routine to your new life. They ask: "What’s changing?" Then they adjust your reminders, suggest backup plans, and even help you talk to your doctor.
If you use an app, make sure it lets you:
- Change your schedule on the fly
- Add notes like "I’m moving Friday - need refill by Wednesday"
- Set alerts for doctor visits or pharmacy changes
Otherwise, you’re just adding another notification to the noise.

What Doctors Should Be Asking - But Often Aren’t
The American College of Physicians now recommends that doctors ask patients one simple question during every visit: "Are you going through any big changes in your life right now?"
Most don’t. But if they did, they’d catch 63.7% of adherence risks before they happen. A 2023 study found that patients who got a transition-specific plan from their provider were 3.2 times more likely to stay on track.
So if you’re about to move, start a new job, or go through a breakup - don’t wait for your doctor to ask. Bring it up. Say: "I’m going through a big change. I’m worried I’ll forget my meds. Can we make a plan?"
Ask for:
- A 30- to 90-day supply so you don’t have to refill during chaos
- Written instructions for your new routine
- A contact person at the pharmacy who can help if you’re in a new city
These aren’t luxuries. They’re safety nets.
Real Stories, Real Results
u/MedAdherenceWarrior on Reddit shared: "I started a new job with 60-hour weeks. I was missing doses. I sat down with my doctor. We broke my regimen into two smaller chunks: one after breakfast, one after dinner. I set alarms tied to my lunch and dinner breaks. In one month, my adherence jumped from 62% to 94%."
Another user, u/TransitionStruggles, wrote: "After my divorce, I stopped my meds for three months. No one asked how it affected me. I didn’t realize I needed help until I got sick. Now I have a plan. My doctor gave me a printed checklist. I check it every Sunday. I’m stable again."
These aren’t outliers. They’re examples of what happens when you stop trying to "just remember" and start building systems.
What to Do Right Now
If you’re in the middle of a transition - or about to be - here’s your action plan:
- Make your three lists. Write down what you can control, influence, and let go of.
- Anchor your meds. Link them to one daily action you won’t skip (brushing teeth, eating, using the bathroom).
- Set up one backup. Keep a 3-day supply in your bag. Give a spare key to a trusted person.
- Call your doctor. Say: "I’m going through a change. Can we make a transition plan?"
- Find one person. Someone who will text you once a day: "Pill taken?"
You don’t need to fix everything. Just keep the most important thing going. One pill. One day. One anchor. That’s enough.
Why do I forget my meds during big changes?
Your brain is overwhelmed. Major life changes trigger stress responses that reduce focus and decision-making power. Routine is tied to environment - when your environment shifts, your automatic habits break. It’s not laziness. It’s biology. The solution isn’t to try harder - it’s to rebuild your cues and supports.
Are reminder apps enough?
Not during transitions. Apps work well in stable times, but during upheaval, they’re buried under other demands. You need human connection, flexible routines, and physical backups - not just alerts. Apps that adapt to life changes (like TransitionAdhere) perform better, but even they work best when paired with a personal plan.
What if I can’t afford a new pharmacy or medication?
Talk to your doctor or pharmacist. Many clinics have patient assistance programs. Some drug manufacturers offer free or discounted meds during hardship. You can also ask for a 90-day supply to reduce refill trips. Never stop meds because of cost - ask for help first.
How long does it take to rebuild a routine?
Most people adapt in 2-3 weeks with focused effort. The first week is the hardest - that’s when you’re most distracted. Set up your anchors, backups, and support system early. After that, consistency builds naturally. You’re not starting from scratch - you’re adapting what already worked.
Can stress really make my meds less effective?
Stress doesn’t make the medication itself less effective. But it makes you less likely to take it - and that’s the same as if it didn’t work. Plus, chronic stress can worsen the condition you’re treating (like high blood pressure or diabetes). So skipping doses during stress creates a double hit: less treatment + more disease pressure.
Ray Foret Jr.
March 8, 2026 AT 21:01Samantha Fierro
March 9, 2026 AT 08:49Robert Bliss
March 10, 2026 AT 13:38Peter Kovac
March 12, 2026 AT 11:01APRIL HARRINGTON
March 13, 2026 AT 13:29Leon Hallal
March 13, 2026 AT 19:55Judith Manzano
March 14, 2026 AT 15:08rafeq khlo
March 14, 2026 AT 17:14Morgan Dodgen
March 15, 2026 AT 00:36Tom Sanders
March 16, 2026 AT 18:48